Written by Dr Mike Armour
Many women with endometriosis report that they find their pain and other symptoms, like fatigue or nausea, are still bothersome, even with medication and sometimes even after surgery. Our research has found that women often report that they become their own ‘health care manager’ and try and manage their symptoms through a multi-disciplinary approach, including medical, surgical, and, in almost 75% of Australian women with endometriosis, using non-pharmacological or complementary therapies.
Complementary medicine (CM), sometimes called complementary and alternative medicine (CAM), is an umbrella term that covers a whole range of therapies and remedies that are not considered to be part of mainstream medical care. This seems pretty straightforward but it does mean that what is a complementary medicine changes depending on where you are in the world, and also over time. For example, in China, acupuncture and Chinese herbal medicine would be considered part of mainstream medicine, as they are delivered in a hospital setting alongside ‘western’ medicine. However in Australia, most would consider acupuncture to be ‘complementary’ despite it having been practiced by some GPs and even occasionally used in hospitals. Similarly, over time, what is ‘complementary’ changes. An example of this would be mindfulness meditation, which would have been considered more a spiritual than medical practice for many years but is now often recommended by doctors as part of stress or mental health management. So it’s tricky to say what is, and isn’t, a “complementary medicine”. For this blog post, we will consider that pretty much everything that isn’t a medical or surgical intervention in Australia might fall under the ‘complementary medicine’ heading, just so we don’t let anything slip through the cracks.
We will look at three major areas where research looks specifically at treating women with endometriosis and is relevant to Australia: complementary therapies (usually where someone does something too you, like an acupuncturist, or massage therapist), complementary medicines or remedies (like herbal medicine) and lifestyle interventions (like dietary changes, or exercise).
Complementary therapies
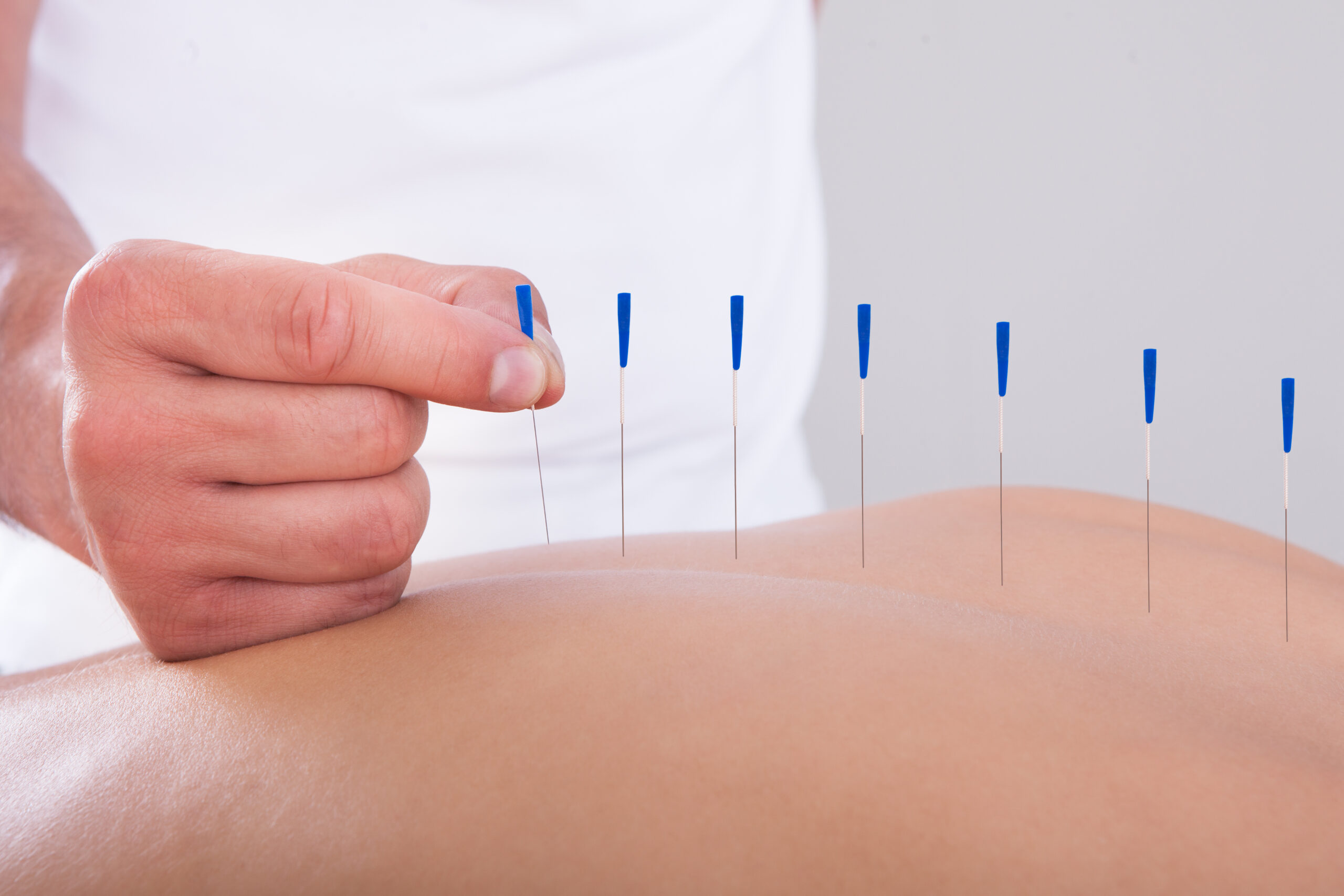 The modality that has the most evidence in this area is acupuncture. There have been several studies on acupuncture for endometriosis pain as an addition to normal treatment. The largest of these used traditional Chinese medicine style acupuncture and found that twice weekly acupuncture treatment significantly reduced pain after 10 weeks. Our research (manuscript in preparation – more information here, found that twice weekly treatment for 8 weeks (16 treatments in total) reduced pain scores by around 50% compared to having no treatment. We also found that is improved overall quality of life scores with women feeling better emotionally and more able to cope with their symptoms. Our study was small, but combined with other, larger studies, there seems to be enough support for acupuncture that it may be worth trying for many women. We found that most women who were going to respond to treatment felt a reduction in pain within 8 treatments (4 weeks). We know that in other conditions, like depression, the total number of treatments and the frequency of treatment are important contributors to the outcome , so if you are planning on trying acupuncture, it might be worth trying to see a practitioner once to twice a week for 3-4 weeks to see if it might benefit you. Acupuncture is generally safe when delivered by a trained practitioner, so it’s very important to make sure your practitioner is qualified so check they are AHPRA registered.
The modality that has the most evidence in this area is acupuncture. There have been several studies on acupuncture for endometriosis pain as an addition to normal treatment. The largest of these used traditional Chinese medicine style acupuncture and found that twice weekly acupuncture treatment significantly reduced pain after 10 weeks. Our research (manuscript in preparation – more information here, found that twice weekly treatment for 8 weeks (16 treatments in total) reduced pain scores by around 50% compared to having no treatment. We also found that is improved overall quality of life scores with women feeling better emotionally and more able to cope with their symptoms. Our study was small, but combined with other, larger studies, there seems to be enough support for acupuncture that it may be worth trying for many women. We found that most women who were going to respond to treatment felt a reduction in pain within 8 treatments (4 weeks). We know that in other conditions, like depression, the total number of treatments and the frequency of treatment are important contributors to the outcome , so if you are planning on trying acupuncture, it might be worth trying to see a practitioner once to twice a week for 3-4 weeks to see if it might benefit you. Acupuncture is generally safe when delivered by a trained practitioner, so it’s very important to make sure your practitioner is qualified so check they are AHPRA registered.
Complementary medicines
There is some research, mostly out of China, that looks at various types of traditional Chinese medicines for endometriosis. Unfortunately, most of the research isn’t great quality, so we can’t be certain at this stage how effective many of these treatments are. There has been a small study that showed individualised Chinese herbal medicine did have positive effects on pain and quality of life, but this trial had problems with the control group so its hard to draw strong conclusions. We (and others) are currently doing research on the effectiveness of herbal medicine for endometriosis, so we hope that in the next year or two we will have more evidence on what herbal interventions might work.
It’s important to remember that herbal medicines or dietary supplements, just because they maybe be natural are not risk free. Many herbal medicines have side effects, and also can interact with medication that you may be taking, so it’s important to discuss any potential use of these with your doctor to make sure there aren’t any potential issues.

Lifestyle interventions
There is some evidence that a particular diet, called the FODMAP diet which limits intake of common foods such as garlic, onions, dairy, apples, legumes (like chickpeas), and a lot of grains (such as wheat), can reduce some of the gastrointestinal symptoms (some of which can fall under ‘Endo Belly’) that women with endometriosis often suffer from. This is quite a restrictive diet, and is only meant for relatively short term use, rather than a lifelong ‘diet’. You can find out more information about the FODMAP diet here. There is also some preliminary evidence that reducing or removing gluten from the diet can also reduce pain. There is a fabulous overview about diet and endometriosis here.

What about exercise?

A very small study on yoga found that 90 minutes of yoga, twice a week, for two months helped reduce pain levels compared to no treatment. Given that yoga may reduce symptoms such as depression, which is often present in women with endometriosis, it may be worthwhile trying yoga. We know from our research that women often reported that yoga could cause them to experience a flare up in their symptoms. Yoga (like most other lifestyle interventions) may work well for some and not for others, depending on then location and severity of your endometriosis lesions, as well as the kind of yoga you chose. So if you are planning on trying out yoga, its probably worthwhile speaking to a qualified yoga therapist about the poses and style(s) that might best suit you, rather than just joining an online class or something with less personalisation. You may also need to try several different styles to find something that suits you personally.
There isn’t much research on more moderate or high intensity exercise on endometriosis symptoms, and exercise was reported to quite frequently cause pain flare ups. Given exercises many health benefits, if you are able to exercise, even if it’s just a short walk, it’s probably worth giving it a go. If you want to do more vigorous exercise but find you just feel worse, it might be worth speaking to a professional, such as an exercise physiologist, on how to do some graded exercise that suits you. Again, like most things, you might find that you just need to tailor this to your symptoms.
So what to do?
This post just covers a few of the more common complementary medicines and lifestyle interventions that might benefit women with endometriosis. Unfortunately, most of the research is based on relatively small studies, so it’s hard to make strong recommendations. However, if you are finding that your symptoms aren’t being controlled by your current treatments, and you want to try adding something to your current treatment regime, then acupuncture, dietary changes, or yoga might be something to try, given the current evidence. Importantly, these additions to your care program have few (but not no) risk and do come at a cost. Just as for medicines and surgery, if these additions are not working for you, then stopping them would be the appropriate course of action.